
PUA 63rd Annual Convention –
Plenary Session 3 : MINIATURIZATION OF PCNL
Miniaturization of PCNL was taken to spotlight on the third Plenary session of the 63rd Philippine Urological Association, Inc. (PUA) Annual Convention 2020, in cooperation with the Philippine Alliance for Urolithiasis (PAU). The session began with an inaugural address by the PAU President and past PUA Chairman, Dr. Jesus Benjamin Mendoza, and was moderated by Dr. Gavino Mercado.
The keynote speakers from the Philippines, China and India imparted their knowledge and experiences to this growing and blooming field of Endourology. Beyond sharing their expertise, the history, indications and advancement towards its applicability were discussed. The program comprised of 4 lectures and 2 panel discussions.


The 1st lecture was entitled, Defining Miniaturization of PCNL, delivered Dr. Michael Conrad Mendoza. His lecture was organized to 3 parts, beginning with (1) Development of the Technique, (2) Evolution of Instruments, and (3) Advancement in Energy used to fragment Stones. He began with the history of PCNL, from the first nephroscopy by Rupel and Brown in 1941 to how it was well-established in 1978 after the collaboration of Dr. Arthur Smith and Kurt Amplatz, paving the way to a paradigm shift in the management of renal stones. Considering the complications of PCNL, he emphasized on significant bleeding and renal damage, as backed by CROES Global PCNL Study in 2011. The evolution of instruments highlighted the development of the PCNL to more advanced techniques of miniperc, micro PCNL, and ultra mini PCNL (UMP). Size does matter according to him, as it is an important factor in reducing intraoperative bleeding and complication in PCNL, hence makes the advantage of miniaturization as an alternative to ESWL and RIRS. His take home message for the audience was, “There is no one better technique. What’s best is what works for you, that you’re comfortable with and is safe for your patients.”


A Panel discussion entitled, How Miniaturization Changed my Practice, moderated by Dr. Enrique Ian Lorenzo follows. He was joined by the following proponents of mini PCNL and local experts in PCNL: Dr. Samuel Vincent Yrastorza, Dr. Albert Aquino, Dr. Karl Marvin Tan, and Dr. Joseph Michael Ursua. Most of them admitted skepticism and doubts with this technique. However, soon after being exposed and trained first-hand by international experts, they soon gain confidence and was slowly incorporated to their practice. As Dr. Yrastorza emphasized, all of them also agreed that openness to learn this new technique is very important. The deciding factors for patient selection and which type of PCNL is applicable are stone burden, Hounsfield units (whether hard or not), location of stones, pre-morbid condition of the patient and complexity of the case. Nobody should be confined to only 1 technique, our choice should remain to be for the best interest and outcome for the patient. Moving forward, when complications are met (in example peritoneal leakage managed by placement of drain, increased irrigation leading to sepsis), Dr. Aquino encouraged all attendees not to be afraid to confront it, but rather recognize and learn from it. Seek help and call a friend if necessary, then pay it forward by sharing and teaching to your colleagues and residents. Dr. Ursua concurs that this is part of the learning curve and be humbled with the experience.
The innovator of mini PCNL himself, Dr. Janak Desai shared his time for a live lecture on Ultra-mini PCNL (UMP). He shared his journey in promoting miniaturization of PCNL. For him, UMP takes a sweet spot between PCNL and RIRS, applicable for stones 15-20mm in size. He focused on comparing UMP with PCNL and flexible ureteroscopy (fURS). He presented a series of published articles focusing on miniaturization. Reducing with UMP having a smaller sheath and tract, there is less onslaught of renal parenchyma to a low as 56% upon reducing the size from 30Fr to 20Fr, more so with a 13Fr in UMP. He even revealed that dilating with a 30Fr actually results to a bigger dilatation of 35Fr with the Amplatz sheath (10x the UMP). He also adds body habitus as a factor, with Asians being smaller, only 9.5-11.5Fr access sheath can be used to up 52% of patients, but is only 40% when increased further to 14Fr. PCNL is a known standard for achieve high Stone-free rate (SFR) for stone management, however, the its downside comes with high complication rates. He did not also dismiss that fURS also share its own complications. Cost and procedure time is also lower with UMP than RIRS. The re-procedure rate is miniscule in UMP (=5%) compared to PCNL (8%) and fURS (100%). The only limiting factor only with UMP is the learning curve, but it is no big deal to learn the art of puncture. UMP boasts of the following advantage: no transfusion, no angio-embolization, may be done on a single session, less hospital stay, and less cost for the patient. As stone experts, we are dependent on all these modalities (PCNL, UMP, RIRS and ESWL). Invasiveness should be tailored according to stone complexity. Science doesn’t go ahead with long leaps, it moves in small incremental steps, and mini PCNL/ UMP is one small but a sure step. He leaves us with a challenge, “UMP is a product of developing technology, so when technology supports us, why cant we take advantage of it?”

The innovator of super mini PCNL (SMP) himself, Dr. Guohua Zeng, came after with his lecture entitled: “Super Mini PCNL for Renal Stones: Techniques and Indications”. For PCNL, bleeding and vascular injury is minimized by puncturing from the fornix, and never from the infundibulum and miniperc techniques such as UMP and SMP. But problems with mini perc techniques were also identified such as: lower irrigation flow brought about by the small access and irrigation channel, difficulty in extraction of stone fragments, compromised endoscopic view and high intrarenal pressure. He showed a video on how these problems are dealt with. With the new generation SMP system, his instruments have an irrigation-suction sheath system. The sheath herein has 2-layered metal sheath, with a tiny gap in-between for irrigation, while 8 holes are at the tip of the sheath for outflow. A pressure vent is present on the handle to control the negative pressure. The RPP for the new-generation SMP is measured at 20.02 +/- 3.58 mmHg. The indications for SMP are stones less than 3cm, failed ESWL or RIRS, and pediatric patients resistant to ESWL. He presented their paper comparing Mini-PCNL and SMP, and results showed that SMP had higher SFR, higher tubeless rate, less complications, less hospital stay for 2-3cm renal stone, equivocal for 3-4cm, but inferior if beyond 4cm. He supplemented it with sample cases showing good outcomes after SMP. In summary, he quoted the chairman of EULIS, Dr Sarica’s definition of SMP as SMP- Safe, Meaningful and Practical.

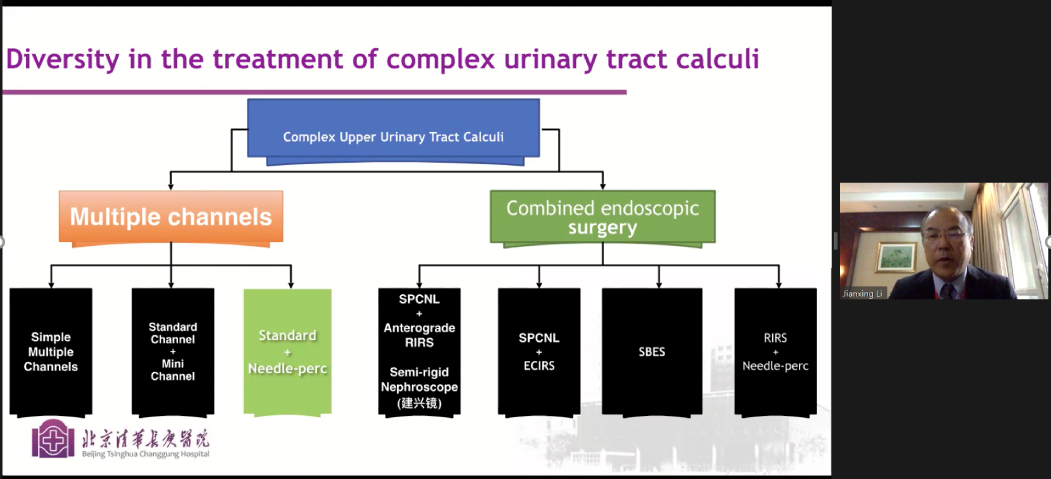
The innovator of needle PCNL himself, Dr. Jianxing Li gave his lecture entitled, A new model for the Treatment of Complex Upper Urinary Tract Calculi (Standard + Needle PCNL). He provided an algorithm on the management of Complex Upper Urinary Tract Calculi, subdivided into multiple channels and combined endoscopic surgery (see image below). Intraoperative irrigation pressure of <30mmHg may be an important factor in preventing post-op sepsis. The number of channels is also an independent factor for increased risk of bleeding and deterioration of renal function as supported by studies, in the expense of high SFR with standard channel PCNL. Advantages of Needle-perc are reduced anesthesia requirement, less injury, less radiation, less risk in patients with solitary kidney and bleeding diathesis (e.g. hemophilia). Needle -assisted PCNL may allow the needle in pushing the stone and reduces the need for multiple tracts. He was able to present its applicability in multiple cases such as complex multiple calculi in a solitary kidney, cystine stones, and with transplanted kidney cases. He ended with his lecture with his take home message that provided a new era where there is already diversity in treatment of calculi, ECRIS and S+N model could gradually take place of some multi-access PCNL, and that Combined S+N model is safe, efficient and economical.

The Panel discussion was short but engaging and fruitful. They all agreed that that one must first master the standard PCNL before venturing and further training for these techniques. A question raised on the timing or deciding factor/parameter of when to stop when faced with difficulty were answered accordingly such as: prolonged operative time (e.g. 90 minutes in Needle-assisted PCNL) and intraoperative patient’s condition. Preoperative planning also is very important so that we do not run into complication. If bleeding is significant, nephrostomy tube may be placed and then come back after. Rare possibility of bowel injury/ puncture must also prompt the surgeon to halt the procedure. They have varied answers when asked whether they use pure fluoroscopy or in combination with ultrasound, however the combined approach has its advantages and indications. It’s a matter of expertise and safety of the patient. Closing remarks was then given by the vice president of PAU, Dr. Pedro Lantin III.
Mabuhay ang PUA! Stay safe everyone.




0 Comments